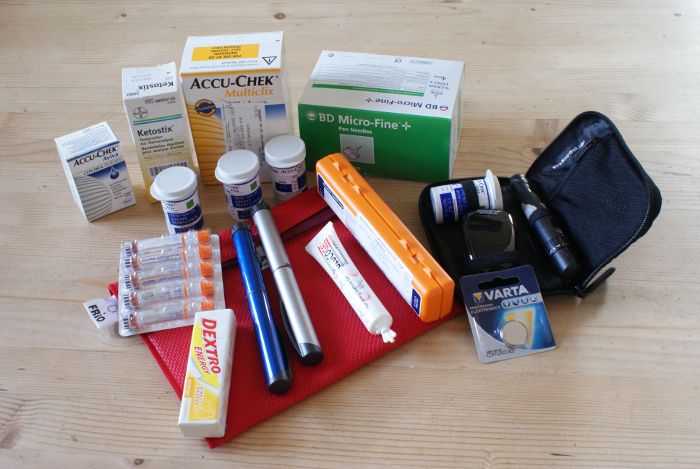
In late July 2011, exactly 7 months after Amy was diagnosed with type 1 diabetes, we backpacked around India for four weeks, in a trip we called Monsoon Meandering.
This is post 13 in the series about that trip and its planning and how type 1 diabetes played a part.
This post is all about how diabetes did or didn’t affect our trip. It’s a summary of what’s been written in some of the previous articles, but here’s it’s all in one place.
This is the last India article from myself as I’m going to let Amy, our type 1 diabetes daughter, summarise the trip and all it meant to her. Her article will be up quite soon.
My memory fades
The India articles are a retrospective view as we went on that trip in August 2011 and here I am writing about them 18 months later. I have wondered whether my mind has forgotten certain details, ones that could be crucial to a person with diabetes attempting travel to India but having triple-checked my facts I hope I’ve got everything correct and moreover covered everything needed by someone thinking of doing a similar trip.
A successful trip?
Fading memory or not I can say that the trip was a huge success.
Diabetes did not stop us doing the trip.
Diabetes did not hinder us through the trip.
Yes, we had the think about things a little and we certainly had to carry more stuff with us on a day to day basis, as we do in the UK.
The biggest problem
Without a shadow of a doubt the biggest problem we faced was running out of Dextrose glucose tablets.
Yes really, that was the biggest problem and one that’s so easily prevented and one that turned out to be easily solved.
I’d done some research beforehand and it seemed that everywhere would have them but we just couldn’t find anything similar in India in the places we looked. We looked in pharmacies, we looked in supermarkets, in hole-in-the-wall stores but nothing. The only glucose we could find was in tubs used by gym-goers.
In the end we just “borrowed” sugar cubes from places we had dinner or drank tea and carried them in the hypo kit.
Changing bolus injection timing
The other spanner which really threw us was Amy’s decision a few days into the trip that she didn’t like Indian food anymore. This really took us by surprise and it took us a while to realise what was going on.
Her decision manifested itself in a few hypos early on which happened because she was injecting before the meal for what she expected to eat but then only eating a bit of it. We switched to injecting after the meal, after we’d seen exactly how much she did eat. This resolved the hypo problem.
Timing of meals
At home we try to make sure meals are around a similar time each, something we’ve only done since Amy got diabetes.
In India we really (,really!) let this slip and it’s something we should have worked harder to keep control of but it was difficult as we were meeting friends and families we didn’t know very well.
A good example of this were when on the first Sunday we were taking out to lunch and a friend of mine wanted to take us to a very popular South Indian restaurant in Connaught Place, one of Delhi’s very popular areas. It was crowded and we eventually go in at 2pm, eating at 2:45pm. That night we had been invited to another friend’s house for dinner and we were probably being too polite when they asked when we’d like dinner, with us saying that we were happy with whenever they wanted. In the end we didn’t start eating until 10pm, way after Amy had taken her basal (Levemir) injection. On reflection we should have explained the situation to them, they would have understood.
Worries about missing injections
In the first few days our bodies’ time clocks were completely out. The first 3 days saw Jane, Emilia and Amy all waking up so late that the first meal of the day was lunch, within 30 minutes of them waking. Consequently, Amy missed out on breakfast and the associated injection, but did this matter? At the time it made sense that if you don’t eat you don’t need a bolus injection to counteract the carbohydrates you haven’t eaten. I’m sure this isn’t a good idea for the long term but over short time period it seemed more appropriate than waking Amy up to eat a breakfast she didn’t want/need at a time when her body needed more rest.
The heat
We really expected the heat to affect Amy’s blood sugars but in all honesty she was the one least affected. On one particular day I found it difficult to keep going and it was Amy who spurred me on. Amy did have a hypo in the middle of a hot day in the middle of a market and we wondered if this was the shape of things to come, but it wasn’t, it was just one of those things which happens in the UK too. We’d already walked a fair bit that day so it was probably tiredness.
Heat did not affect her.
Injections on trains
Amy’s forthcoming article will talk about this in more detail but in summary she found a method of injecting on the trains which got over her fear of injecting when the world around her is not completely still: we simply timed our meals to coincide with stops at stations.
Finally, I’ll leave you with a photo of my favourite place from that trip.